Abstract
Purpose
To evaluate the diagnostic potential of PET/MRI with [18F]FDG in recurrent ovarian and cervical cancer in comparison to PET/CT.
Methods
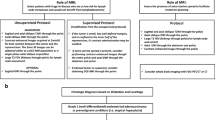
A group of 19 patients with suspected recurrence of pelvic malignancies (ovarian cancer, 11 patients; cervical cancer, 8 patients) scheduled for an [18F]FDG PET/CT were subsequently enrolled for a PET/MRI. The scan protocol comprised: (1) a T1-W axial VIBE after contrast agent adminstration, (2) an axial T2-W HASTE, (3) a coronal TIRM, (4) an axial DWI, and dedicated MR sequences of the female pelvis including (5) a T1-W VIBE before contrast agent adminstration, (6) a sagittal T2-W TSE, and (7) a sagittal T1-W dynamic VIBE. The datasets (PET/CT, PET/MRI) were rated separately by two readers regarding lesion count, lesion localization, lesion conspicuity (four-point scale), lesion characterization (benign/malignant/indeterminate) and diagnostic confidence (three-point scale). All available data (histology, prior examinations, PET/CT, PET/MRI, follow-up examinations) served as standard of reference. Median values were compared using the Wilcoxon rank sum test.
Results
Metastatic lesions were present in 16 of the 19 patients. A total of 78 lesions (malignant, 58; benign, 20) were described. Both PET/CT and PET/MRI allowed correct identification of all malignant lesions and provided equivalent conspicuity (3.86 ± 0.35 for PET/CT, 3.91 ± 0.28 for PET/MRI; p > 0.05). Diagnostic confidence was significantly higher for PET/MRI in malignant (p < 0.01) and benign lesions (p < 0.05).
Conclusion
Both PET/CT and PET/MRI offer an equivalently high diagnostic value for recurrent pelvic malignancies. PET/MRI offers higher diagnostic confidence in the discrimination of benign and malignant lesions. Considering the reduced radiation dose and superior lesion discrimination, PET/MRI may serve as a powerful alternative to PET/CT in the future.




Similar content being viewed by others
References
Koh W, Greer BE, Abu-Rustum NR, Apte SM, Campos SM, Chan J, et al. Cervical cancer. J Natl Compr Cancer Netw. 2013;11:320–43.
Takekuma M, Maeda M, Ozawa T, Yasumi K, Torizuka T. Positron emission tomography with 18F-fluoro-2-deoxyglucose for the detection of recurrent ovarian cancer. Int J Clin Oncol. 2005;10:177–81. doi:10.1007/s10147-005-0489-6.
Sironi S, Picchio M, Landoni C, Galimberti S, Signorelli M, Bettinardi V, et al. Post-therapy surveillance of patients with uterine cancers: value of integrated FDG PET/CT in the detection of recurrence. Eur J Nucl Med Mol Imaging. 2007;34:472–9. doi:10.1007/s00259-006-0251-y.
Brooks RA, Rader JS, Dehdashti F, Mutch DG, Powell MA, Thaker PH, et al. Surveillance FDG-PET detection of asymptomatic recurrences in patients with cervical cancer. Gynecol Oncol. 2009;112:104–9. doi:10.1016/j.ygyno.2008.08.028.
Bipat S, Glas AS, van der Velden J, Zwinderman AH, Bossuyt PMM, Stoker J. Computed tomography and magnetic resonance imaging in staging of uterine cervical carcinoma: a systematic review. Gynecol Oncol. 2003;91:59–66.
Donati OF, Hany TF, Reiner CS, von Schulthess GK, Marincek B, Seifert B, et al. Value of retrospective fusion of PET and MR images in detection of hepatic metastases: comparison with 18F-FDG PET/CT and Gd-EOB-DTPA-enhanced MRI. J Nucl Med. 2010;51:692–9. doi:10.2967/jnumed.109.068510.
Ruf J, Lopez Haenninen E, Boehmig M, Koch I, Denecke T, Plotkin M, et al. Impact of FDG-PET/MRI image fusion on the detection of pancreatic cancer. Pancreatology. 2006;6:512–9. doi:10.1159/000096993.
Schreiter NF, Nogami M, Steffen I, Pape U, Hamm B, Brenner W, et al. Evaluation of the potential of PET-MRI fusion for detection of liver metastases in patients with neuroendocrine tumours. Eur Radiol. 2012;22:458–67. doi:10.1007/s00330-011-2266-4.
Tatsumi M, Isohashi K, Onishi H, Hori M, Kim T, Higuchi I, et al. 18F-FDG PET/MRI fusion in characterizing pancreatic tumors: comparison to PET/CT. Int J Clin Oncol. 2011;16:408–15. doi:10.1007/s10147-011-0202-x.
Kitajima K, Suenaga Y, Ueno Y, Kanda T, Maeda T, Deguchi M, et al. Fusion of PET and MRI for staging of uterine cervical cancer: comparison with contrast-enhanced (18)F-FDG PET/CT and pelvic MRI. Clin Imaging. 2014;38:464–9. doi:10.1016/j.clinimag.2014.02.006.
Kitajima K, Suenaga Y, Ueno Y, Kanda T, Maeda T, Makihara N, et al. Value of fusion of PET and MRI in the detection of intra-pelvic recurrence of gynecological tumor: comparison with 18F-FDG contrast-enhanced PET/CT and pelvic MRI. Ann Nucl Med. 2014;28:25–32. doi:10.1007/s12149-013-0777-6.
Martinez-Möller A, Souvatzoglou M, Delso G, Bundschuh RA, Chefd’hotel C, Ziegler SI, et al. Tissue classification as a potential approach for attenuation correction in whole-body PET/MRI: evaluation with PET/CT data. J Nucl Med. 2009;50:520–6. doi:10.2967/jnumed.108.054726.
Antoch G, Saoudi N, Kuehl H, Dahmen G, Mueller SP, Beyer T, et al. Accuracy of whole-body dual-modality fluorine-18-2-fluoro-2-deoxy-D-glucose positron emission tomography and computed tomography (FDG-PET/CT) for tumor staging in solid tumors: comparison with CT and PET. J Clin Oncol. 2004;22:4357–68. doi:10.1200/JCO.2004.08.120.
Keller F, Psychogios G, Linke R, Lell M, Kuwert T, Iro H, et al. Carcinoma of unknown primary in the head and neck: comparison between positron emission tomography (PET) and PET/CT. Head Neck. 2011;33:1569–75. doi:10.1002/hed.21635.
Freudenberg LS, Rosenbaum SJ, Beyer T, Bockisch A, Antoch G. PET versus PET/CT dual-modality imaging in evaluation of lung cancer. Radiol Clin North Am. 2007;45:639–44. doi:10.1016/j.rcl.2007.05.003.
Scharitzer M, Ba-Ssalamah A, Ringl H, Kolblinger C, Grunberger T, Weber M, et al. Preoperative evaluation of colorectal liver metastases: comparison between gadoxetic acid-enhanced 3.0-T MRI and contrast-enhanced MDCT with histopathological correlation. Eur Radiol. 2013;23:2187–96. doi:10.1007/s00330-013-2824-z.
Kim CK, Park BK, Choi JY, Kim B, Han H. Detection of recurrent ovarian cancer at MRI: comparison with integrated PET/CT. J Comput Assist Tomogr. 2007;31:868–75. doi:10.1097/rct.0b013e31803e8c45.
Barnholtz-Sloan J, Patel N, Rollison D, Kortepeter K, MacKinnon J, Giuliano A. Incidence trends of invasive cervical cancer in the United States by combined race and ethnicity. Cancer Causes Control. 2009;20:1129–38. doi:10.1007/s10552-009-9317-z.
Brix G, Lechel U, Glatting G, Ziegler SI, Munzing W, Muller SP, et al. Radiation exposure of patients undergoing whole-body dual-modality 18F-FDG PET/CT examinations. J Nucl Med. 2005;46:608–13.
Schwenzer NF, Schraml C, Muller M, Brendle C, Sauter A, Spengler W, et al. Pulmonary lesion assessment: comparison of whole-body hybrid MR/PET and PET/CT imaging – pilot study. Radiology. 2012;264:551–8. doi:10.1148/radiol.12111942.
Beiderwellen K, Gomez B, Buchbender C, Hartung V, Poeppel TD, Nensa F, et al. Depiction and characterization of liver lesions in whole body (18)F-FDG PET/MRI. Eur J Radiol. 2013;82:e669–75. doi:10.1016/j.ejrad.2013.07.027.
Buchbender C, Hartung-Knemeyer V, Beiderwellen K, Heusch P, Kuhl H, Lauenstein TC, et al. Diffusion-weighted imaging as part of hybrid PET/MRI protocols for whole-body cancer staging: does it benefit lesion detection? Eur J Radiol. 2013;82:877–82. doi:10.1016/j.ejrad.2013.01.019.
Integrity of research and reporting
All human studies were approved by the local institutional review board and were therefore performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments.
Acknowledgments
This research project was supported by a grant from the German Research Foundation (Deutsche Forschungsgemeinschaft, DFG). LaleUmutlu is a consultant for Bayer HealthCare. The other authors declare no conflicts of interest
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Beiderwellen, K., Grueneisen, J., Ruhlmann, V. et al. [18F]FDG PET/MRI vs. PET/CT for whole-body staging in patients with recurrent malignancies of the female pelvis: initial results. Eur J Nucl Med Mol Imaging 42, 56–65 (2015). https://doi.org/10.1007/s00259-014-2902-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00259-014-2902-8