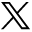Visual Abstract
Abstract
The aim of this study was to assess the rates of undiagnosed diabetes mellitus (DM) and pre-DM in patients undergoing gastric emptying scintigraphy (GES). Diabetes is an epidemic in the United States, and the disease is associated with altered gut motility. As a result, we suspected that a significant number of patients referred for GES may have undiagnosed DM or pre-DM. Given that established procedure standards for GES require all patients to prepare with an 8-h fast, an opportunity is provided to measure the fasting blood glucose (FBG) in all individuals before they undergo the examination. Methods: The charts of patients undergoing GES were reviewed for a history of DM and correlated with FBG and GES results. FBG values, obtained by point-of-care testing, were categorized as normal, pre-DM, or DM. Results: Patients with known DM made up 23% of those referred for GES, and most (55%) had a normal FBG. In those without a history of DM, there were a significant number with undiagnosed pre-DM (12%) and DM (33%). Conclusion: Our study provides the first measure of the likely prevalence of undiagnosed DM and pre-DM and characterizes the different gastric emptying patterns among patients with normal FBG, likely undiagnosed pre-DM, likely undiagnosed DM, and known DM.
- quality assurance
- diabetes
- fasting plasma glucose
- gastric emptying scintigraphy
- gastroparesis
- prediabetes
The diabetes mellitus (DM) epidemic in America is a public health crisis with projections that indicate a continual rise in the coming years (1). Further amplifying the issue is the staggering one third of the total DM population who are undiagnosed and hence untreated (2). The burden of DM is particularly high in certain ethnic groups, such as South Asians living in America, who have a higher prevalence of DM than others (3). Complications associated with DM, including retinopathy, nephropathy, cardiomyopathy, neuropathy, and atherosclerosis, contribute to significant morbidity, mortality, and cost to health care.
Efforts to manage and prevent DM through early identification of pre-DM are routine. The fasting blood glucose (FBG) measured before the start of a gastric emptying scintigraphy (GES) examination is an opportunity to lessen the burden on patients and society.
MATERIALS AND METHODS
Under approval by the institutional review board, we conducted a retrospective chart review of all patients undergoing GES from January 2019 to June 2021 (n = 260). The demographics of the studied population were unique to the diverse group of U.S. military beneficiaries comprising active-duty soldiers, family-member dependents, and veterans. From this initial query, 251 met the inclusion criteria for the study. Each patient’s chart was reviewed for a history of DM and correlated with FBG and GES results. FBG values, obtained by point-of-care testing (StatStrip; Nova Biomedical), were categorized as normal, concerning for pre-DM, or concerning for DM on the basis of the diagnostic criteria defined by the American Diabetes Association (4). GES was performed in accordance with established procedure standards of the Society of Nuclear Medicine and Molecular Imaging and with international accreditation committee guidelines (5,6). Patients with DM were not categorized by type.
RESULTS
Patients with known DM made up 23% of those referred for GES, and most (55%) had a normal FBG. In those without a history of DM, there were a significant number with likely undiagnosed pre-DM (12%) and DM (33%) (Tables 1 and 2; Fig. 1).
GES Results Based on DM Status
Distribution of Abnormal GES Results Based on Diagnosis of DM Vs. FBG in Non-DM Patients
Distribution of GES results based on FBG and whether patient had history of DM.
Approximately half the patients who underwent GES had abnormal results (53%). A higher proportion of those with likely undiagnosed DM than with likely undiagnosed pre-DM had abnormal GES results (75% vs. 50%). Among those with undiagnosed pre-DM and DM, rapid emptying studies were more common than delayed emptying studies. Likely undiagnosed DM patients had an average FBG of 166 mg/dL with a maximum FBG of 263 mg/dL. There were 5 undiagnosed patients with an FBG of more than 200 mg/dL, which exceeds the recommend cutoff for GES as defined by the Society of Nuclear Medicine and Molecular Imaging guidelines.
DISCUSSION
The clinical impact of FBG before GES is twofold. In patients with normal gastric emptying results, FBG can be used to screen DM or pre-DM. And for those with abnormal gastric emptying results, FBG can be used to characterize the patient’s delayed GES as likely DM or pre-DM gastroparesis rather than idiopathic. The impact of these findings is significant given the high volume of GES examinations performed each year.
Public Health Impact
A significant number of patients referred for GES likely have undiagnosed pre-DM or DM (45%). This statistic is not surprising given that an estimated third of all patients with DM in the United States are undiagnosed and that DM is the number one cause of gastroparesis. The potential clinical impact of detecting these cases of undiagnosed DM or pre-DM is significant given the large volume of GES procedures performed across the country. A 2021 nationwide survey reported that the average nuclear medicine clinic performed about 200 GES procedures per year, with large academic centers performing up to 2,000 annually. These numbers were limited to just 121 of 872 potential medical institutions who responded to the survey (7).
Improved Accuracy of Fasting Plasma Glucose (FPG) Compared with Hemoglobin A1C (HbA1c) When Screening for DM or Pre-DM
The use of FPG as a screening test will improve detection of pre-DM or DM in patients who have already been screened. Many patients referred for GES will have already been screened for DM with the less sensitive test HbA1c instead of the more sensitive FPG or 2-h oral glucose tolerance test. HbA1c is more commonly ordered because of its greater convenience (no fasting required) and performance as a marker of chronic hyperglycemia; however, its sensitivity is poor and differs between ethnicities. HbA1c will diagnose only 30% of cases, many of which would have been detected by FPG. The glucose tolerance test is an alternative screening and diagnostic test. This test is uncommonly ordered because of its logistic barriers but is the most sensitive for both pre-DM and DM, outperforming FPG and HbA1c (2,8). Collectively, each of these tests can categorize patients into normal, pre-DM, or DM status but evaluates different pathophysiologic processes within the broader diagnosis of dysglycemia. Abnormal FPG denotes impaired fasting glucose with a primary deficiency in insulin secretion. In contrast, an abnormal 2-h oral glucose tolerance test reflects impaired glucose tolerance from abnormal insulin resistance (9).
A review of the current literature on our studied population within the military health system reveals similar findings. Although our study included family members and retirees, poor screening practices among those on active duty within the U.S. military across all branches presents an opportunity for an even greater clinical impact. Clutter et al. reported that roughly 50% of all service members met criteria for screening (>45 y old or 18–25 y old with a body mass index > 25 kg/m2) but only 6% were screened (10).
More Accurate Identification of DM or Pre-DM Gastroparesis
The high rates of undiagnosed pre-DM or DM result in significant clinical implications due to potential mischaracterization of the type of gastroparesis. If patients referred for GES have already been screened with HbA1c and the results were negative, then an abnormal GES may not be properly attributed to diabetic gastroparesis. Instead, the patient’s delayed gastric emptying may be labeled as idiopathic gastroparesis, which has an extensive list of potential causes, including medications, infectious disorders, autoimmune disorders, neurodegenerative disorders, and other functional gastrointestinal disorders (11).
Rapid Gastric Emptying as an Early Indicator of Pre-DM
Multiple studies have shown a potential relationship between rapid gastric emptying and early type 2 DM. It is possible that rapid gastric emptying may be one of the earliest indicators of abnormal postprandial hyperglycemia before abnormal screening by FPG, glucose tolerance testing, or HbA1c. Our results demonstrate a significant number of patients with rapid gastric emptying and normal FBG, and it is possible that this subgroup of patients may progress to pre-DM and should be monitored (12).
Implementation of Routine FBG Before GES
Preimaging FBG is built into the standard workflow of GES at our institution and presents an opportunity to screen for DM or pre-DM in patients referred for suspected gastroparesis. Our results suggest that nuclear medicine imaging centers should routinely perform FBG before GES and, more importantly, document the results in the impression. This should be considered in addition to the reporting recommendations in the GES guidelines. Language such as “FBG of X is concerning for DM or pre-DM and warrants further testing with FPG or a 2-h oral glucose tolerance test to confirm” should be used. Unfortunately, long-standing poor adherence to current GES procedure standards suggests a significant barrier to implementation (13).
CONCLUSION
This study highlights the diagnostic implications of undiagnosed DM or pre-DM in patients referred for GES detected through FBG screening. The high prevalence of likely undiagnosed DM or pre-DM in this population emphasizes the need for early detection and intervention. The identification of impaired fasting glucose during GES not only allows for the identification of likely DM or pre-DM but also provides insights into the underlying causes of delayed gastric emptying, allowing for differentiation of DM or pre-DM gastroparesis from idiopathic gastroparesis. The public health impact of screening for undiagnosed DM or pre-DM in patients referred for GES is significant, given the large volume of GES procedures performed annually. Additionally, the use of FBG as a screening test improves the accuracy of DM or pre-DM detection compared with HbA1c, and the necessary preparation is already built into the standardized workflow for GES as recommended by societal guidelines. Furthermore, the high prevalence of rapid gastric emptying in patients with normal FBG may serve as an early indicator of pre-DM in certain high-prevalence populations. Implementing routine FBG assessment before GES can aid in the early identification and management of DM or pre-DM and diabetic gastroparesis.
DISCLOSURE
No potential conflict of interest relevant to this article was reported. The Department of Defense and Defense Health Agency do not necessarily endorse, support, sanction, encourage, verify, or agree with the comments, opinions, or statements contained herein.
KEY POINTS
QUESTION: What are the rates of undiagnosed pre-DM and DM in patients undergoing GES?
PERTINENT FINDINGS: 45% of patients undergoing GES had FBG concerning for undiagnosed DM or pre-DM.
IMPLICATIONS FOR PATIENT CARE: The implementation of universal FBG for all patients undergoing GES provides an excellent opportunity to screen for a prevalent and debilitating disease that remains markedly underdiagnosed and undertreated.
Footnotes
Published online Feb. 13, 2024.
REFERENCES
- Received for publication October 9, 2023.
- Revision received January 5, 2024.